




Dear reader,
Six billion people worldwide lack access to safe, timely, and affordable cardiac surgical or interventional services when needed. Cardiovascular diseases remain the world’s leading cause of mortality with nearly 18 million deaths per year, yet a sole focus on prevention remains the cornerstone of global health interventions.
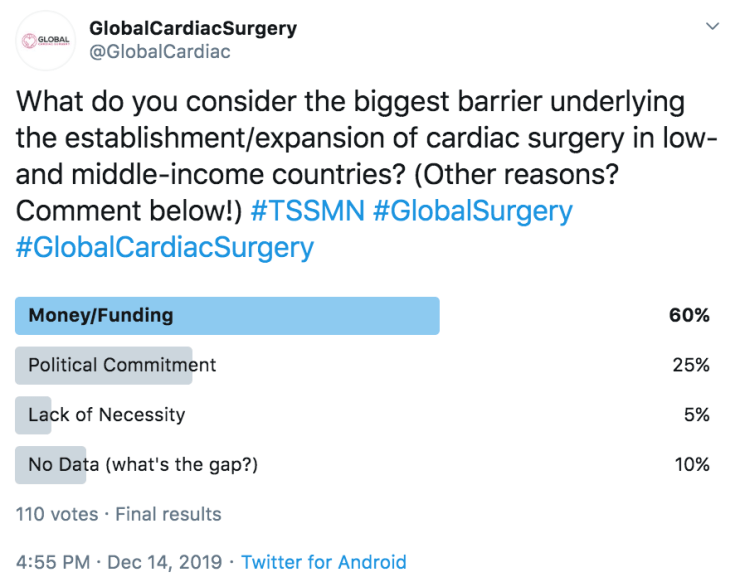
Through the following short (5-minute) survey, we want to assess the proportion of cardiovascular diseases requiring surgical or interventional care, as opposed to medical or conservative treatment.
We would greatly appreciate your expert opinion and thank you in advance.
Survey: https://forms.gle/RFm7TRKacPzbSQ1h7
Questions or concerns can be sent to Dr. Dominique Vervoort at vervoortdominique@hotmail.com
From September, 18th to October, 1st 2018, the 73rd edition of the United Nations General Assembly (UNGA) took place at and around the United Nations Headquarters in New York, United States. The UNGA is one of the six main organs of the United Nations, the only one in which all Member States have equal representation, during which Heads of State and international institutions discuss and vote upon resolutions regarding all issues affecting the world and covering all Sustainable Development Goals (SDGs).

Health discussions, once again, took up a large part of the UNGA agenda, in particular during UNGA side events around New York. Although official Global Surgery meetings and contributed panels were limited (G4 Alliance’s “Eradicating Neglected Surgical Diseases: Advancing Universal Health Coverage Through Surgical Systems Strengthening” and the Access Challenge‘s Universal Health Coverage Conference), attention for the indispensable role of surgery to tackle non-communicable diseases (NCDs) gained increasing attention.
On September, 25th, Partners in Health, NCD Synergies, and the Program in Global NCDs and Social Change at Harvard Medical School held the breakfast event “What will it take to address NCDs and injuries (NCDI) for the poorest billion? Leading with equity on the NCDI and UHC agendas” at the Harvard Club of New York City. Here, attention was raised for the need to address NCDs and injuries in the poorest populations, given the disparities in accessing care. Different from many other events, however, a patient voice was included on the panel.
Erneste Simpunga, a young man from Rwanda, survived near-fatal rheumatic heart disease (RHD). He was diagnosed with RHD at the age of 16, and slowly progressed into heart failure. He needed valve replacement surgery, but there were no cardiac surgeons in Rwanda. His parents never finished high school and already sold many assets just to allow him to go to school. His family did not have tens of thousands of dollars to send him abroad for surgery. Even then, follow-up care would be an issue. “In Rwanda, we only have 6 cardiologists for 12 million people. Although our country has made great progress in health insurance, health workforce shortages remain an incredibly limiting barrier in accessing care.“, he said. After receiving philanthropic aid to fly to Boston and receiving life-saving surgical care, he is now in his fifth year of medical school at the University of Rwanda in Kigali, Rwanda, aspiring to become a cardiologist or cardiac surgeon and help his country in a way he could not be helped domestically. However, hundreds of thousands of babies are born with congenital heart disease, and hundreds of thousands children and adults suffer from rheumatic heart disease in Rwanda – many millions around the world, all waiting for life-saving surgery.
 Ernest Simpunga (second from right): “Surgery in India would cost 15,000 dollars, which we could not afford, and it would take three years for visiting teams to treat me. Seeing cardiologists and taking medicines costed hundreds of dollars per month, so I had to change to a cheaper high school.“
Ernest Simpunga (second from right): “Surgery in India would cost 15,000 dollars, which we could not afford, and it would take three years for visiting teams to treat me. Seeing cardiologists and taking medicines costed hundreds of dollars per month, so I had to change to a cheaper high school.“
On the evening of September, 25th, the American Heart Association, in collaboration with NCD Synergies, Partners in Health, Children’s HeartLink, and other partner organizations, hosted the “Time to Disrupt the Health Care System: Novel Solutions for Quality Care in the SDG Era” event, listening to patient advocates and global champions in advancing prevention and care for cardiovascular diseases (CVD). Here, surgical voices as Erneste, as well as Dr. Bhagwan Koirala (cardiac surgeon from Nepal) and Jackie Boucher (President of Children’s HeartLink) raised the notion of surgical care to treat CVD.
 Dr. Koiral (third from left): “Highly specialized, but widely needed care such as cardiac surgery can efficiently be provided in low- and middle-income countries with effective care models. In Nepal, we treat patients from neighbouring countries due to our low costs for cardiac surgery.“
Dr. Koiral (third from left): “Highly specialized, but widely needed care such as cardiac surgery can efficiently be provided in low- and middle-income countries with effective care models. In Nepal, we treat patients from neighbouring countries due to our low costs for cardiac surgery.“
On September, 27th, the Third United Nations High-Level Meeting (HLM3) on Non-Communicable Diseases brought together Heads of State and leading non-governmental organizations to discuss the current state of NCDs and (re-)prioritize frameworks to address these around the world. Although Heads of State continued to repeat the message of traditional prevention focus in tackling NCDs, Dr. Sania Nishtar, Co-Chair of the WHO High-Level Commission on NCDs, underlined the importance of surgery to address the global rise in morbidity and mortality due to NCDs: “While designing universal health coverage, we must also cater to the poorest billion. We must recognize that access relates not just to medicines, but also to surgery given that 5 billion individuals lack access globally.“
A long way is still to go to achieve equivocal attention for the link between surgery and NCDs, especially for cardiac surgery and cardiovascular diseases. The need for the global community to open up to wider discussions and understand the importance of intersectoral and interdisciplinary collaborations (read “Global Cardiac Surgery: a Wake-Up Call” for a longer note) is urgent and will determine the course of efforts towards UHC and the SDGs in 2030.
Article by Ulrick S. Kanmounye Email: ulricksidney@gmail.con
One might wonder why it is important for the Democratic Republic of Congo (DRC) to have cardiothoracic surgical services. First and foremost, the DRC has an estimated 77.8 million inhabitants, most of whom are poor. This means there is a need for 23,340 cardiac surgeries per year (Zilla et al. Unpublished data). Secondly, the country has been the theatre of wars, Ebola and cholera epidemics, tuberculosis, HIV, and malaria endemics. These infectious diseases have diverted attention and resources to the detriment of surgery in general and of cardiothoracic surgery in particular. The two aforementioned reasons also explain the high prevalence of rheumatic heart disease among Congolese children. Finally, congenital heart diseases (CHD) are a major public health issue in this country. According to data from the Kinshasa University Clinic, during the early 2000s, an estimated 2,000 children were born with CHD yearly in the capital city Kinshasa. Therefore, there is an urgent need for cardiac surgery equipment, interventions, and workforce in the DRC.
The evolution of cardiac surgery in the DRC has known three distinct phases. The first phase was characterised by the practice of cardiac surgery by Belgian surgeons and a lack of Congolese cardiothoracic surgeons. This phase began back in 1956 when the University of Kinshasa (formerly known as Lovanium) was run in partnership with Belgians from the Free University (Université Libre). Teams of cardiothoracic surgeons from Belgium would travel to Kinshasa and perform closed-heart surgeries. Fifteen years later, things changed when the first Congolese cardiothoracic surgeons returned home. First in 1970, with Dr André Beloy (Kinoise Clinic and Ngaliema Clinic) and later on in 1971 with Pr Joseph Kabemba (Kinshasa University Clinic). Then came the second phase which was marked by a major recession of cardiothoracic activities. This phase lasted more than 30 years. During this era a few professors did their best to keep cardiothoracic activities going but they faced too many difficulties. These were Professors Kabemba, Kiula, Mushegera, and Muteba. Unaided, their efforts were not sufficient to maintain cardiothoracic activities. Finally, towards the end of the first decade of the 2000s, a few Congolese doctors took upon themselves to make things change. It is this collective movement that constitutes the last phase. During this period, Congolese doctors from within and from without the borders of the DRC have organised themselves in groups to rekindle the light of Congolese cardiothoracic surgery.
There are two major groups of doctors that have contributed to this new cardiothoracic era. The first of both groups is the NGO “Les Chaines de l’Espoir RD Congo”. This NGO is made up of Pr Shiku Diayisu (Cardiopaediatrician – Kinshasa University Clinic), Dr Nyakabasa Mutijima (Paediatrician – Ngaliema Clinic) and Dr Etienne Tshionyi (Surgeon – Ngaliema Clinic). Together, they have been able to operate 120 children in the DRC (Patent Ductus Arteriosus and first phase of Tetralogy of Fallot) and 70 children in Belgium with the help of Pr Jean Rubay (Université Catholique de Louvain). The greatest achievement has been the construction of a 2 million USD cardiopaediatric centre at the Ngaliema Clinic site. They were able to achieve such a fit thanks to the sponsorship of the first lady of the DRC, Mrs Olive Kabila. This centre has 2 operating rooms: one for open-heart surgery and another for neurosurgery. To perform these interventions, a team of 8 Ngaliema Clinic staff went to Christian Barnard Memorial Hospital, Cape Town where they were trained by Dr Susan Vosloo. Once they returned in 2017, the team performed open heart surgeries on two patients (Ventricular Septal Defect and Mitral Valve Replacement). Despite major financial support, both patients found it difficult to pay the remaining 300 USD for their interventions. Unfortunately, no other interventions have been performed since then.

Ngaliema Clinic Cardiopaediatric Centre
The second group is an Association of Alumni of the University of Kinshasa’s Medical School (AFMED – Association des Amis et Anciens Eudiants de la Faculté de Médecine de Kinshasa). Two diasporan members of AFMED have been operating patients at the Monkole Hospital Centre and Kinshasa University Clinic during the summer. These two are Dr Alphonse Nzomvuama (Cardiothoracic Surgeon – France) and Dr John Nsiala (Anaesthesiologist – France). Together, they have operated nine Patent Ductus Arteriosus and two Chronic Constrictive Pericarditis between 2012 and 2015. In addition, AFMED works outside the operating room as it organises a yearly conference during which Congolese doctors from all around the world come together to share their experiences with their local colleagues. During the first AFMED conference in 2012, Dr Nzomvuama talked about the current state and future of cardiothoracic surgery in the DRC. He has been to major local television and radio stations every year to call for changes in local health policies.
Cardiac surgery was once the spearhead of Congolese medicine. Today, it is struggling to re-establish itself. Fortunately, a lot has been done locally by doctors to shake things up. These modern day heroes are not equipped to win this battle. However, they will stand a chance if they receive help from fellow colleagues and global surgery advocates.